Blockers and the brain
Kids' hospital gender clinic tells families the effect of puberty blockers on the brain is unknown

The gist
Parents and patients at Australia’s biggest children’s hospital gender clinic have been told that the effects of puberty blocker drugs on the brain are unknown.
The latest newsletter from the gender clinic at Royal Children’s Hospital Melbourne (RCH) informs families of a new research project to try to work out whether these drugs, used to suppress the natural sex hormones of an unwanted puberty, also have effects on the still maturing adolescent brain.
The RCH gender clinic has given public assurances that transgender hormone suppression is “reversible”. The claim that puberty blockers are a low-risk “pause” in development has come under challenge internationally.
Puberty blocker medication is typically started early in puberty — around ages 9-13 — with the stated purpose of relieving the distress of gender dysphoria in children who declare a trans or non-binary identity and want to stop the development of sex characteristics such as breasts or facial hair.
Puberty blockers are often promoted as “life saving” but systematic reviews of the medical literature on gender dysphoria conclude the evidence on the effects of these drugs is low quality, inconclusive or missing.
The RCH gender clinic’s newsletter, sent to families on June 1, includes an outline of a new PhD study under the heading “Puberty blockers and the brain”.
The research outline says suppression of natural sex hormones “might conceivably delay brain development.
“On the other hand, it might help to facilitate normal brain development, since use of puberty blockers in trans adolescents is associated with improvements in mental health.”
The outline says it is unclear whether the natural hormones of puberty have a role to play in adolescent changes to the brain.
“Related to this, we do not know whether using puberty blockers affects development of the brain,” the newsletter says.
The brain is not fully mature until the mid-late 20s. It is unknown whether there are critical windows of time for maturation processes of the brain to take place, or whether catch-up in cognitive development is possible when patients move from puberty blockers to cross-sex hormones.
The PhD research project at the RCH clinic is to track the brain function of two groups of adolescents over time, those who take puberty blockers and those who do not.

The detail
The planning for this RCH research project appears to date back at least to 2019 when the gender clinic — and its research partners at the Murdoch Children’s Research Institute and the University of Melbourne — advertised for an interested postgraduate student.
The clinic appeared confident that natural sex hormones would be shown to affect the developing adolescent brain.
“Puberty is a time of rapid change within the brain. Whilst the biological basis for this change remains uncertain, changes in sex hormones, such as oestrogen and testosterone, likely play an important role,” the advertisement said.
“Many of our patients [at RCH] are treated with medication to block the production of pubertal hormones in order to prevent their bodies developing in a way that is incongruent with their inner gender identity.”
The research proposal was to set a range of cognitive tasks for patients undergoing puberty blockade and compare their results with a matched control group of local school students.
“This use of puberty blocking medication typically occurs for several years and provides an opportunity to learn how the teenage brain develops in the absence of sex hormones.”
Journalistic digging
Last month, the flagship investigative TV program of Sweden’s public broadcaster, Mission: Investigate, was awarded a prestigious “Golden Spade” journalism prize for its coverage of the risks of youth gender medicine.
The most recent of its “Trans Train” documentary series broadcast claims that Sweden’s biggest youth gender clinic — part of the renowned Karolinska University Hospital — failed to detect injury and harm done to children on puberty blockers.
The program said about 440 children with gender dysphoria had received puberty blockers from 2015 to 2020, and noted the policy to limit the duration of treatment to minimise risks and side-effects such as low bone density.
Paediatric endocrinologist Dr Ricard Nergårdh, a senior clinician at the Karolinska, replied “We don’t know” when asked, on camera, how long was too long to be on puberty blockers, but added that international guidelines suggested a two-year maximum.
Mission: Investigate said it had uncovered data showing that 87 children had been on puberty blockers for more than three years, thereby increasing the risk of side-effects such as low bone density and fractures.
The program featured a 15-year-old patient, “Leo”, who was diagnosed with osteopenia — a brittle-bone condition usually seen in the elderly — after four and a half years on puberty blockers.
Dr Nergårdh, who was using hormone suppression within the “Dutch protocol” of medicalised gender change to try to ease the distress of vulnerable children, said the evidence for the effectiveness and risks of these medical treatments was “relatively weak”.
“I’m very worried about it,” he told Mission: Investigate. “ And I think I’m not alone in that.”
“What we call GnRH treatment, or puberty blockers, is chemical castration,” he said. “And it can affect mental health in an unintended, undesirable way. So it’s very important that the patient and the patient’s family are informed of this.”
GnRH treatment — with gonadotropin releasing hormone analogues — is also used with endometriosis in women, advanced prostate cancer in men, and to suppress libido in sex offenders.
There is no long-term safety data on hormone blockade of young people with gender dysphoria, but women with endometriosis on GnRH treatment report menopause-like side-effects such as hot flashes, night sweats, mood changes and weight gain.
For prostate cancer patients, the Canadian website Life on ADT tracks research on hormone blockade referred to in this domain of healthcare as androgen deprivation therapy.
Studies suggest these cancer patients run the risk of metabolic syndrome, depression and cognitive impairment.


The Gray Lady plays catch-up
On Wednesday, The New York Times magazine published an article “The Battle Over Gender Therapy” by staff writer Emily Bazelon, who updated readers on disagreement and recrimination within the coterie of “gender-affirming” clinicians.
She touched on early puberty blockade followed by cross-sex hormones and the resulting risks to fertility and the capacity for sexual relationships when these children become adults.
Clinicians are advised to discuss “future unknowns related to sexual health” under a December 2021 draft of the new treatment guideline from the World Professional Association for Transgender Health.
“Little is known about the impact [of puberty blockers] on brain development,” Bazelon reported.
The current, 2012 WPATH guideline claims that blockers are “fully reversible”.
In October last year, American journalist Abigail Shrier asked trans clinician Dr Erica Anderson, the immediate past president of the US Professional Association for Transgender Health, if she believed the psychological effects of blockers were reversible; the reply was: “I’m not sure”.
Bazelon’s reporting suggests a divide between more cautious gender clinicians — who insist on comprehensive assessment and are uncertain about the surge in teenagers seeking trans medical interventions — and the radicals who are uncompromising about what they see as a trans health rights issue.
The December draft WPATH guideline attributes at least some of the exponential increase in adolescent gender patients to “social influence” online or via peer groups.
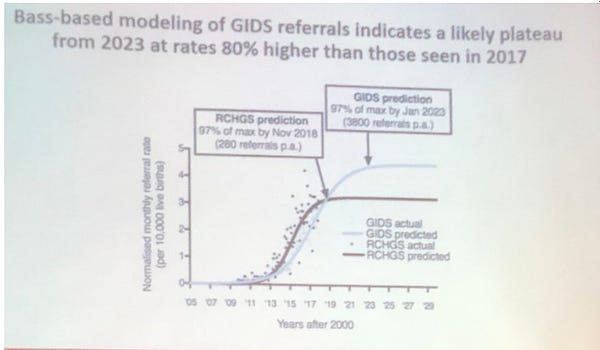
The Times article cited a 2020 British-Australian study reporting a correlation between 2,614 media items on the trans topic and spikes in new referrals at RCH in Melbourne, and the Tavistock youth gender service in the United Kingdom.

Bones, not brains
The 2018 guideline issued by the Royal Children’s Hospital Melbourne has been promoted as the first specific set of treatment recommendations for children and adolescents diagnosed with gender dysphoria. It does away with minimum age thresholds for hormonal treatment, advising individualised decision-making by clinicians.
The guideline, which is used by other Australian children’s hospital gender clinics, does not discuss the issue of puberty blockers and the brain, but appears to assume that brain development is unaffected by hormone suppression.
It says thinner bones are “the main concern” with early suppression of the natural sex hormones which promote bone density.
The document claims that puberty suppression “is reversible in its effects” and gives a young patient “time to develop emotionally and cognitively prior to making decisions on gender-affirming hormone use which [has] some irreversible effects”.
In last year’s Australian Story profile on ABC TV, the RCH clinic director, Dr Michelle Telfer, said: “Puberty blockers are reversible. The only risk is that it can affect your bone density.”
On the limited data available, almost all patients started on blockers proceed to irreversible opposite-sex hormones.
Critics of gender-affirming medicine suggest that puberty blockers may lock-in discomfort with birth sex and set children as young as age 9 on a path to lifelong medicalisation with implications beyond their capacity to understand or consent.
Some gender clinicians, however, now argue that near universal progression to cross-sex hormones in fact vindicates the selection of children started on puberty blockers, suggesting a stable opposite-sex identity and a low risk of treatment regret.
This implies contradictory rationales for puberty blockers, according to Australian paediatrician Dr Dylan Wilson.
“Which is it? Either puberty blockers are ‘reversible’ and give children ‘time to think’ or puberty blockers are the right first step along the pathway for the children they have definitely selected to be the right candidates to be transgender adults,” Dr Wilson says in a new Substack post debunking the “myth” of reversibility.
Backpedalling on reversibility
The effect and purpose of puberty blockade was a key issue in 2019-22 litigation against the U.K. Tavistock youth gender clinic, which is part of the National Health Service (NHS). Senior judges were split on what conclusions could be properly drawn.
In mid-2020, with no announcement, the NHS updated its gender dysphoria webpage, and abandoned its former claim that puberty blockers were “fully reversible”.
New disclaimers were added to the webpage, stating that blockers are “physically reversible if stopped [but] it is not known what the psychological effects may be.
“It’s also not known whether hormone blockers affect the development of the teenage brain or children’s bones. Side effects may also include hot flushes, fatigue and mood alterations.
“Little is known about the long-term side effects of hormone or puberty blockers in children with gender dysphoria.”
In 2019, a letter from British paediatrician Dr Christopher Richards and two health profession colleagues was published by the journal Archives of Disease in Childhood under the heading “Use of puberty blockers for gender dysphoria: a momentous step in the dark”.
“… puberty blockers are now being used in the context of profound scientific ignorance. The causes of gender dysphoria are largely unknown as are the reasons for its rapidly changing epidemiology [from very few early-onset natal males to very many adolescent-onset females],” the letters’ authors say.
They say that the longstanding endorsement of puberty blockade for central precocious puberty — a condition occurring in girls before age 8 or boys before age 9 — does not resolve questions about the safety of these drugs when used with dysphoric youth.
“It is surely presumptuous to extrapolate observations from an intervention that suppresses pathologically premature puberty to one that suppresses normal puberty,” they say.
“To halt the natural process of puberty is an intervention of momentous proportions with lifelong medical, psychological and emotional implications. We contend that this practice should be curtailed until we are able to apply the same scientific rigour that is demanded of other medical interventions.”
In April this year, the interim report from U.K. Cass review of gender dysphoria care cited the 2020 “Consensus parameter” paper in which 24 international experts in fields including neurodevelopment and adolescence collaborated to identify the key research questions necessary to elucidate the effects of puberty blocking on cognition and the brain.
“The pubertal and adolescent period is associated with profound neurodevelopment, including trajectories of increasing capacities for abstraction and logical thinking, integrative thinking (for example, consideration of multiple perspectives), and social thinking and competence,” the paper says.
“The combination of animal neurobehavioural research and human behaviour studies supports the notion that puberty may be a sensitive period for brain organisation: that is, a limited phase when developing neural connections are uniquely shaped by hormonal and experiential factors, with potentially lifelong consequences for cognitive and emotional health.”
The complex research project outlined by the paper — involving multiple gender clinics and more than one comparison group — is yet to begin.
Paperwork
An RCH informed consent document, dated July 2019 and obtained under freedom of information law in 2020, requires parents to declare: “I understand that the effects of [puberty blocker drugs] are reversible. This means that if my child chooses to stop hormone treatment, their pubertal development will start again.”
Neither this RCH document, nor the patient information sheet (dated April 2019), states that the effect of puberty blockers on brain development is unknown. They do carry a general disclaimer that “There may be risks of [puberty blocker] treatment that are not yet known”.
The informed consent document also requires parents to say they “understand that the medical effects and safety of long-term use of [puberty blockers for gender dysphoria] are not fully understood and there may be long term risks that are not yet known.
“However, there is a long history of their use in children with early onset [or precocious] puberty without serious side effects.”
Hormone blocker drugs are approved for use with precocious puberty so that the premature development of these young children can be put on hold until they can join their peer group going into normally timed puberty.
The same drugs are used “off-label” with gender dysphoria — they are not approved for this use — and their effect is to suspend the normally timed puberty of patients while their peers continue to develop.
On the RCH informed consent document, the child gives “assent” to puberty blocking and states “[I] believe I understand the potential benefits and side-effects of [puberty blocker] therapy.”
The clinician declares that he or she is “satisfied” the child “understands the nature of the proposed treatment and the consequences of both the treatment in terms of intended and possible side-effects and also the possible consequences of failure to treat”.
RCH did not reply when asked if these patient documents had been updated.
Overload
In a September 2021 snapshot, the RCH gender clinic had a total of 1,120 patients receiving treatment ranging from mental health support through speech pathology to hormonal interventions. The year before, only 538 patients were being treated.
In the year 2012, when Dr Telfer became director, the clinic had 18 new referrals. In 2021, there were 821 new referrals.
Earlier this month, the gender clinic wrote to families of older children on its waiting list saying they would be transferred to the adult gender clinic at Monash Health in Melbourne.
The letter says that although the adult clinic “also has a waiting time of more than 12 months, it is not as long as that currently being experienced [at RCH]”.
The letter raises the option of families seeking a private specialist.
In a 10-year audit of the RCH clinic, published last year, 23 per cent of a sub-group of 234 patients were given puberty blockers with “just a single patient stopping this treatment without progressing to [cross-sex hormones]”. Of this sub-group, 20.5 per cent received cross-sex hormones.
The audit data may not represent the overall patient profile and treatment rates of the clinic with its more recent period of dramatic growth, the removal of legal obstacles, increased funding, and trans promotion through schools and media.
The audit covers from 2007-16. In its early years, the clinic was quiet, with only 82 new referrals from 2007-13. Demand took off in the mid-2010s, with 1,831 new referrals from 2014-20.
In 2010, the Labor government in the RCH clinic’s home state of Victoria launched the “trans-inclusive” Safe Schools program with its Queer Theory-style content teaching that biological sex and an inner sense of “gender identity” can be at odds.
In 2013, it became easier for Australian gender clinicians to prescribe puberty blockers following a test case, re Jamie, in which the Family Court was told by the federal human rights commission that “the consequences of making a wrong decision [to give blockers] are not grave”.
The court noted evidence that the treatment was “fully reversible, without long-term effects on fertility”. An endocrinologist, identified only as “Dr G” under secrecy provisions imposed by the judges, claimed puberty blockers had “no side-effects”.
In 2015, the RCH gender clinic was given new funding of $6 million over four years, enabling it to hire more staff and pay for puberty blockers, which are not subsidised by the federal Pharmaceutical Benefits Scheme.
In 2017, the Family Court liberalised access to cross-sex hormones. A year later, the court ruled it was no longer necessary to seek judicial approval for under-18 trans surgery, unless there was disagreement between doctors or parents.
Major media promotion of the clinic began in 2014, towards the end of the audit period, with the ABC TV Four Corners program “Being me”.
In 2019, a Victorian royal commission into mental health was told that “many” of the previous year’s intake of natal female patients at the RCH gender clinic were requesting “chest reconstructive surgery” (or mastectomy, also known as ‘top surgery’).
“[RCH] does not currently have the resources to support chest reconstructive surgery although it does have the surgical expertise to carry out this procedure”, clinic director Dr Telfer said in her evidence.
“There are also no private surgical services available for [trans] adolescents under the age of 18 years in Victoria, leaving them with no option but to seek chest reconstructive surgery interstate or overseas should they be unable to manage their distress until they turn 18 years of age.”
In a statement to The Australian newspaper last year, RCH said it “does not currently offer ‘top surgery’.”
Asked if gender clinic patients had been referred by RCH to private surgeons, the hospital said it was “not aware of any referrals of gender service patients to private surgeons for ‘top surgery’ or other gender affirming surgery”.
Note: Questions were put to RCH, Dr Telfer, and the Murdoch Children’s Research Institute.
GCN does not dispute that gender-affirming clinicians believe their interventions are of benefit to vulnerable patients in distress. In a 2019 statement, RCH said its gender clinic treatment was based on the “best available medical evidence”, in line with “international best practice”, and followed “strict clinical governance standards”.




Thank you again!
Indeed:"Bazelon’s reporting suggests a divide between more cautious gender clinicians — who insist on comprehensive assessment and are uncertain about the surge in teenagers seeking trans medical interventions — and the radicals who are uncompromising about what they see as a trans health rights issue."
However that is not the only divide- Sweden's Karolinska's hospital restricted new treatments of minors to clinical trials. More restrictive than both of these groups, which by no means span all the expert opinion or what the evidence supports.
That is, there are indeed two groups which advocate two approaches to medical intervention in the US, but it is by no means the case that this is the whole debate. Given the weak evidence, many clinicians find the wpath guidelines not cautious enough. See segm....